June 17, 2021
-Politico
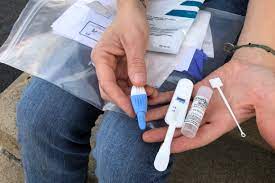
The pandemic brought widespread Covid testing into people’s homes. Now, public health officials across the country are seeing whether the convenience and privacy of similar easy-to-use kits can help them track the spread of sexually transmitted disease.
As society reopens, officials in Los Angeles, Washington, D.C. and even rural Idaho are mailing thousands of free HIV test kits to people who request them online — and are starting to do the same for STDs. With gonorrhea, chlamydia, syphilis at record high rates, the officials say new self-swab and finger-prick testing options that patients mail to labs could ease pressure on strapped public health clinics, still consumed with the coronavirus crisis, that also bear the burden of more routine disease surveillance.
Washington, D.C.’s city government has shipped nearly 2,000 STD test kits since last summer and reports a roughly 6 percent positivity rate among those returned — significantly higher than in-person clinics were reporting before the pandemic. Many of those individuals had not been tested before and weren’t showing symptoms.
“These are people who wouldn’t otherwise know they have an STD,” said Michael Kharfen, a senior deputy director at the DC Department of Health.
But regulatory obstacles and concerns over cost and human error could keep the at-home tests from becoming the new norm. Most tests designed for at-home sample collection haven’t been authorized by the Food and Drug Administration. And their effectiveness hinges on patients figuring out how to use them. Samples that sit too long in the mail or are exposed to either very hot or very cold temperatures could yield false positives, or worse, not detect actual cases. And while some health departments are contracting with established test-makers and private labs, the online market for STD tests has become a wild west, with startups making unsubstantiated claims as they market directly to patients.
“Regulation has to catch up to clinical practice,” said Jennifer Mahn, associate director for clinical programs at the National Coalition of STD Directors. “The stakes are too high here.”
FDA officials declined to say how they’re treating the growing at-home test market or what applications are pending. The agency said in a statement it will “continue to balance our role of protecting and promoting public health while supporting medical device innovation.”
Public labs either have to go through a time-consuming and costly process of validating tests that aren’t authorized by the FDA, or leave the job of evaluating samples to the private labs that developed the tests — which can cost as much as 10 times more. And while most public labs lack the staff, time and equipment to undertake that validation process, particularly as they continue to process thousands of Covid tests, those labs that have begun to look at the new STD tests are concerned about what they’ve found.
“Several of our members who are in the process of validating these tests have found that you lose sensitivity and reliability when you collect samples at home,” said Kelly Wroblewski, the director of infectious diseases at the Association of Public Health Labs. “What kind of a loss in performance are you willing to accept for the convenience of home collection?”
The STD tests also fall into a regulatory gray area, with different federal agencies overseeing the kits and the labs that process them. Experts like Barbara Van Der Pol, a professor at the University of Alabama at Birmingham who sits on the board of directors of the American Sexually Transmitted Diseases Association, are urging the FDA to streamline the process so public health labs can take a bigger role.
Van Der Pol said government agencies also should do more to educate the public and crack down on scams as more companies get into the home-testing game.
“People are just putting out tests and making claims about them that aren’t supported,” she said. “There are claims on some of these sites that because they can’t say ‘FDA-approved’ say something like ‘FDA-recognized,’ and an end-user wouldn’t know … ‘recognized’ means nothing.”
Concerns about the new tests extend beyond their regulatory and scientific challenges, to how a patient will respond to a positive result outside the clinic setting.
Officials fear that many people who test positive won’t seek treatment or share information about recent contacts for tracing, potentially allowing diseases to spread unchecked.
“Are we worried about a 15-year-old getting a positive HIV result on their cell phone and not doing any follow up because they don’t know what to do? Yes, we are,” Mahn said. “We’re excited about this as an innovative solution but we’re concerned about losing the relationship with the patient.”
Still, health officials rolling out the new tests in their communities argue they’re meeting a real need and say demand is holding steady even as state and local health departments receive a flood of new federal funding and start to reopen in-person HIV and STD clinics. Not only does in-person testing often require a person to take time off work or find childcare, people accustomed to ordering everything on their phones are increasingly expecting medical care to be equally convenient.
“Honestly, if you had to spend three hours plus transit to get an STD test in a clinic, whereas you could just collect it at home in five minutes, what are you going to do?” asked Van Der Pol, whose home state has some of the nation’s highest rates of chlamydia and gonorrhea, and recently launched its own partnership to provide free home-collection STD kits to anyone over 12 years old.
Idaho’s public health department, which launched a free at-home testing program for HIV and STDs during the height of the pandemic in partnership with the group Building Healthy Online Communities, is hoping test kits can reach at-risk people in the sprawling rural state, where a person may have to travel hours to reach the nearest brick-and-mortar clinic and conservative social attitudes discourage some from visiting sexual health centers or consulting a family doctor.
Pre-pandemic, most Idahoans who tested positive for HIV were getting diagnosed at the most advanced stage, according to Kevin Brinegar, who leads the state’s efforts on HIV, STDs and Hepatitis.
“That tells us that access to testing is struggling,” he said. “If people are putting it off until they’re sick, that’s a problem.”
Brinegar says while demand for test kits is lower than expected, they are reaching people who couldn’t or wouldn’t seek testing otherwise and catching infections earlier. He said 41 percent of the people ordering the kits reported never before gotten tested, and many others had not gotten a test in months or years.